A stroke can have a profound impact on a person’s cognitive abilities, affecting memory, attention, executive functions, and processing speed. While cognitive impairment can limit daily independence and reduce quality of life, recent advances in cognitive rehabilitation are offering new hope to survivors. By harnessing the power of neuroplasticity; the brain’s ability to reorganise itself… rehabilitation is moving beyond traditional paper-and-pencil exercises towards a more intensive, personalised, and technology-driven approach. At its core, cognitive rehabilitation is based on two complementary approaches: restorative and compensatory.
- Restorative approaches aim to repair or restore a damaged cognitive function. These techniques often involve repetitive, focused training to stimulate and reorganise neural pathways affected by the stroke.
- Compensatory approaches focus on teaching new strategies and skills to help a person work around their cognitive deficits. This might involve using external aids like memory notebooks or technology to manage daily life.
Digital technologies are now playing a central role in delivering cognitive rehabilitation, offering engaging, interactive, and data-driven therapies.
- Computer-assisted cognitive training (CACT): Software platforms, like BrainHQ and RehaCom, provide structured, game-like exercises that target multiple cognitive domains, including attention, working memory, and processing speed. A recent meta-analysis found that CACT was significantly more effective than conventional methods for improving general cognitive function as measured by the Montreal Cognitive Assessment (MoCA), which heavily emphasises executive function.
- Virtual Reality (VR) and gamification: VR offers a safe, simulated environment for stroke survivors to practice real-world tasks, such as shopping or managing finances. The immersive nature of VR can increase patient motivation and engagement, which is critical for driving neuroplastic change. Studies suggest VR can be more effective than conventional training for improving overall cognitive function, attention, and executive function.
- Telerehabilitation: Using technology to provide rehabilitation remotely is increasing access and allowing for higher doses of therapy in the home or community. This is particularly valuable for patients facing challenges with transport or access to high-quality rehabilitation centres.
Increasingly, researchers are exploring how to combine different types of therapies to maximise recovery.
- Exercise and cognitive training: Combining physical activity, such as aerobic exercise, with cognitive training appears to enhance global cognitive function and memory. Exercise increases cerebral blood flow and levels of neurotrophins, such as brain-derived neurotrophic factor (BDNF), which promotes neuronal survival and plasticity.
- Brain stimulation: Non-invasive brain stimulation techniques, like transcranial magnetic stimulation (TMS) and transcranial direct current stimulation (tDCS), can be used alongside traditional therapies to modulate cortical excitability and promote neuroplasticity. While the evidence is still evolving, some studies suggest that NIBS can enhance the effects of therapy, particularly for neglect and language deficits.
- Integrated cognitive-behavioral training: Recent research highlights the benefits of integrating cognitive training with behavioral strategies. A study in chronic stroke patients found that adding a computer-based cognitive-behavioral training program to a physical therapy regimen significantly enhanced cortical reorganisation and improved performance in memory, attention, and logical reasoning.
While promising, the field of cognitive rehabilitation still faces challenges, including the heterogeneity of stroke and the need for larger, high-quality clinical trials. However, several trends point towards a more effective future:
- Personalised, biomarker-driven care: Tailoring interventions to the individual patient, guided by biomarkers and neuroimaging, could optimise outcomes.
- Multidisciplinary collaboration: Optimising recovery requires seamless cooperation between neurologists, rehabilitation specialists, engineers, and technology developers.
- Leveraging motivation: Designing rehabilitation around engaging, gamified, and ecologically valid tasks can increase patient motivation and adherence, which are key drivers of neuroplasticity.





 Virtual Reality (VR) is transforming monotonous exercises into interactive games, boosting patient engagement and motivation. Studies have shown that when used alongside traditional therapy, VR can significantly improve motor function and quality of life for stroke survivors.
Virtual Reality (VR) is transforming monotonous exercises into interactive games, boosting patient engagement and motivation. Studies have shown that when used alongside traditional therapy, VR can significantly improve motor function and quality of life for stroke survivors. Robotic devices can also supplement therapy by assisting with intensive, repetitive exercises that might otherwise be too demanding for therapists or patients. The best results often occur when robotic therapy is combined with conventional methods, and different robots are suited for varying needs.
Robotic devices can also supplement therapy by assisting with intensive, repetitive exercises that might otherwise be too demanding for therapists or patients. The best results often occur when robotic therapy is combined with conventional methods, and different robots are suited for varying needs. Upper limb exoskeletons operate in several modes to help with different stages of recovery:
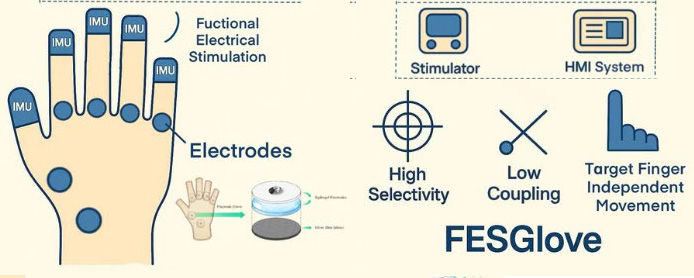
Upper limb exoskeletons operate in several modes to help with different stages of recovery: Functional Electrical Stimulation (FES) uses electrical pulses to activate muscles artificially, helping to practice functional tasks like grasping and reaching. When coupled with voluntary movement, this technique can help promote neuroplasticity, the brain’s ability to reorganize itself. Surface electrodes can be placed on the skin, or in more advanced setups, integrated into electrode arrays on a fabric sleeve or orthosis.
Functional Electrical Stimulation (FES) uses electrical pulses to activate muscles artificially, helping to practice functional tasks like grasping and reaching. When coupled with voluntary movement, this technique can help promote neuroplasticity, the brain’s ability to reorganize itself. Surface electrodes can be placed on the skin, or in more advanced setups, integrated into electrode arrays on a fabric sleeve or orthosis. Wearable sensors take the form of wrist-worn sensors or special gloves can track arm movements and provide real-time feedback through a tablet or app. Gamified devices have also been available for many years. Both the following are produced by long-term colleagues of ARNI: GripAble, is a great example which turns exercises into engaging, fun activities for at-home use. And Neuroball
Wearable sensors take the form of wrist-worn sensors or special gloves can track arm movements and provide real-time feedback through a tablet or app. Gamified devices have also been available for many years. Both the following are produced by long-term colleagues of ARNI: GripAble, is a great example which turns exercises into engaging, fun activities for at-home use. And Neuroball